Pros
Through experimentation, and extending the application of drugs like Metformin that had a positive impact on blood sugar (glucose) levels, the pharma industry has now launched a range of GLP-1 agonists that mimic a hormone in the body and affect various endocrine and digestive processes, with a net result that people feel less hungry less often, and when the do eat, they eat less.
The GLP-1 meds are injectables, either weekly, or daily, and have some side effects, which many people don’t like, but the good news is that they show efficacy against obesity in a way that the scientific-theoretical could not. The trials of Wegovy showed around 15% weight loss over a year.
While I believe the downsides to outweigh the benefits (details below), I fully understand how the pharma weight loss approach will be attractive to many people who have struggled and failed to lose weight many times, who feel dejected, and whose health is suffering.
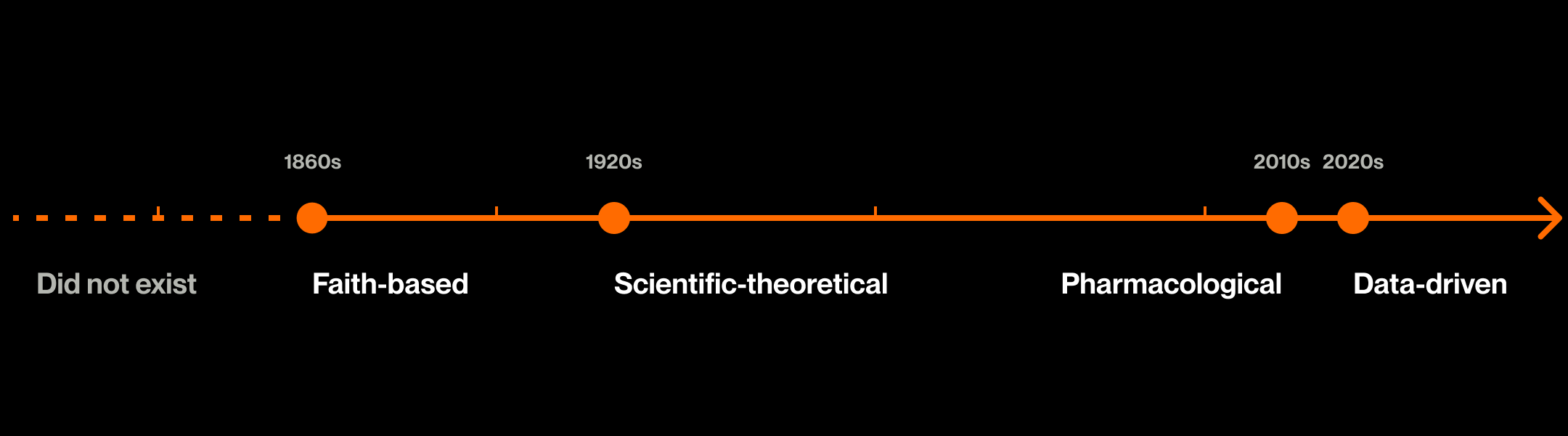
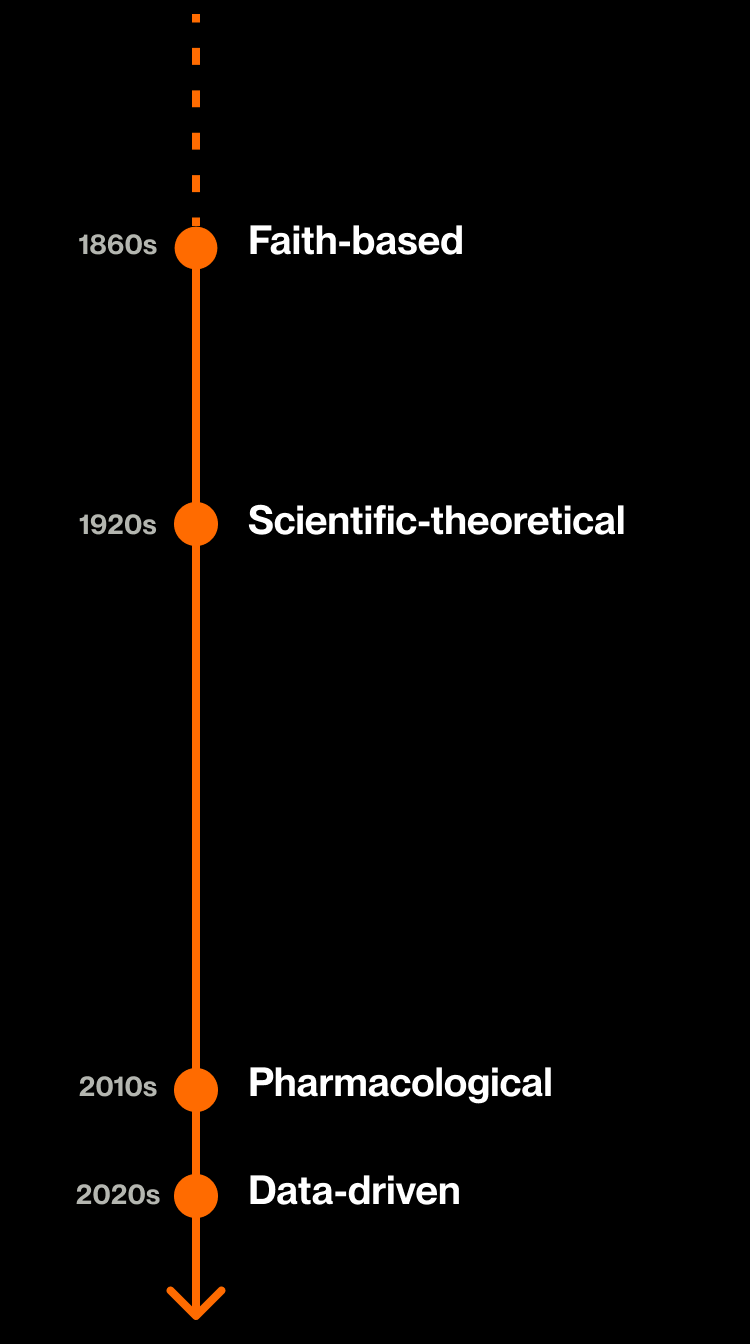
Compared to a heightened risk of diabetes, cardiovascular disease, or other common comorbidities of obesity, the chance to “kick-start” a weight loss process and move out of the “danger zone” is an appealing one, especially given the total failure of the 20th Century's scientific-theoretical approach to weight loss.
Cons
“But what’s not to like?” say many people. I’ll go into detail in another post, but in brief, the main issues are cost, recidivism, short-termism, and side effects. There are also unknown long-term risks, as well as personal factors issues, like frequent injections many people don’t like.
Cost is a major issue, as the list price for Wegovy, the most advanced GLP-1 med on the market, is $1349.02 for a month’s supply. Novo Nordisk offers some discounts in non-US markets, and for those in the US whose insurance does not cover it, but it is very expensive.
It is only temporary salve, and recidivism levels seem to be almost 100%. The very high price is made worse by the fact that you have to take GLP-1 meds forever, or the weight will come back. Because you are injecting an “artificial support” for your satiety systems — you are mitigating the effects of food choices that resulted in obesity, rather than changing those choices — the body, once the artificial support is pulled away, reverts to its prior state. Same behaviors, same end result.
The quick-fix mindset derails real change. Like so much marketing in modern life, the promise of a “quick fix” or a “silver bullet” for obesity has equal and opposite downsides. While pharmacological interventions can dull appetite and slow metabolic processes, they come at a cost of deferring real change and understanding of the body. The only truly long-term, sustainable way to lose weight and keep it off is to gain an understanding of your body, the foods you put in, and the impact those have on you. The quick fix of injections is like using a crutch rather than mending a broken leg.
Side effects and inconvenience can be a barrier. The FDA lists “nausea, diarrhea, vomiting, constipation, abdominal (stomach) pain, headache, fatigue, dyspepsia (indigestion), dizziness, abdominal distension, eructation (belching), hypoglycemia (low blood sugar) in patients with type 2 diabetes, flatulence (gas buildup)” and other side effects, which are perhaps unsurprising when injecting large volumes of hormone agonists.
There are also many unknown long-term risks. There have been no long term studies on GLP-1 injections, including lifetime impact analyses; no study on the vacuum created by forcing a set of physiological reactions in the body, and no pleiotropic impact studies of effects on the biome or other systems. Lastly, as a personal preference, many people don’t like or want to inject themselves with syringes.
The bottom line is that, while unquestionably more effective than the fad diets or false empiricism of the prior, there are significant problems with the GLP-1 medications, and downsides to consider.